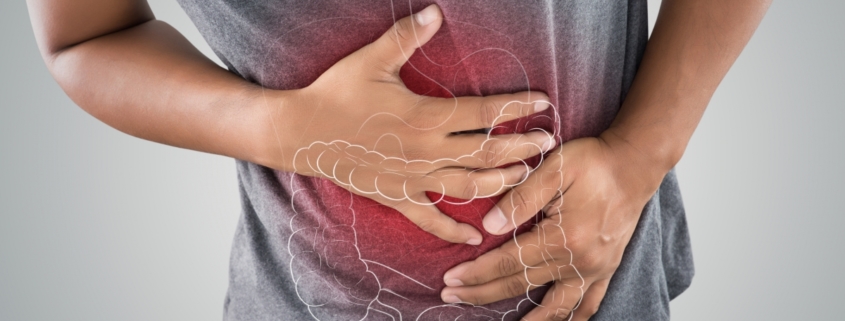
What is Leaky Gut? Could you be suffering from this condition?
Leaky gut syndrome has gained some considerable attention in the health industry, despite still not being entirely recognized by many medical professionals. Leaky gut is the generic term for an abnormally increased intestinal permeability, a medical term for “small holes in the intestines”. This condition results in an abnormal amount of absorption of materials that should not otherwise pass through the intestines and into the bloodstream. Some of the substances that make it through the intestinal barrier may include bacteria, antigens, food particulates and inflammatory mediators which can lead to a host of potential problems. Malabsorption of minerals is another sequele of this condition. Untreated and undetected leaky gut may be responsible for some acute and chronic health conditions. Some of the more common conditions linked to leaky gut include:
- autoimmune diseases
- diabetes
- cardiovascular disease
- multiple bowel-related problems (IBS, IBD)
- weight gain
- psychological conditions
- joint problems
Causes of leaky gut are multi-factorial. Daily stress, non-steroidal anti-inflammatory drugs, alcohol consumption, cow’s milk intolerance, small intestine bacterial overgrowth, pancreatic insufficiency and intestinal infections are all potential sources of inflammation. It becomes quite apparent that intervention is paramount in these cases in order to break the cycle, restore gut health and ideally result in resolution of the associated conditions present.
Assessment strategies for leaky gut syndrome appear to be open to interpretation at the present time. It is largely a diagnosis that is made clinically through the presence of some key indicators.
These key indicators are symptoms such as:
- bloating
- gas
- constipation
- diarrhea
- fatigue
- headaches to name a few.
When a patient presents in my office, I am sure to assess their medical and social history, dietary habits and medication use as these areas can provide keen insights into presence and severity of the condition. Additional assessment tools that are often used to assist in diagnosis are the IgG food intolerance test and the urinary indican test. The indican test is an indicator of intestinal toxemia and bacteria. Normally urinary indican should be quite low, where elevated levels can signify maldigestion and malabsorption of protein. Keeping in mind that other conditions can raise urinary indican levels such as hypochlorhydria, stomach cancer, insufficient digestive enzymes, malabsorption syndromes, SIBO, intestinal obstruction. If it is high in the correct context without more severe pathology present, it can be a useful indicator of a leaky gut.
IgG food intolerance testing is another popular and widely consumed test that measures the immune system activity in response to the presence of certain foods in the diet. IgG, commonly associated with type 3 hypersensitivity reactions, is a chronic inflammatory marker that can provide insight into how much and what types of foods are triggering an inflammatory response. When removing foods that test strongly positive on IgG testing, one is removing an agent directly contributing to inflammation, whether it be the initial cause or a contributing factor. Once an IgG food intolerance testing has been ordered and adequately interpreted, guidance can be more uniquely tailored to the individual patient. These tests can measure up to 220 types of food antigens present in blood as well as the degree of the inflammatory response elicited. It can be a valued assessment tool as previously discussed and also be used to construct unique diet plans.
The typical leaky gut protocol is one that is rich in antioxidants, fiber, mucosal nutrients, fermented foods, is balanced and avoids food sensitivities. If you think this approach will benefit you, reach out for more information. Happy to help you restore your gut and life!
In good health,
Dr. Jennifer Cisternino, Naturopath
416-301-3477




Leave a Reply
Want to join the discussion?Feel free to contribute!